Unstable Ankle Following an Ankle Sprain
ANKLE CONDITION
A twisting injury or going over on the ankle usually results in an inversion of the foot and ankle. This produces a spectrum of injuries to the lateral ankle.
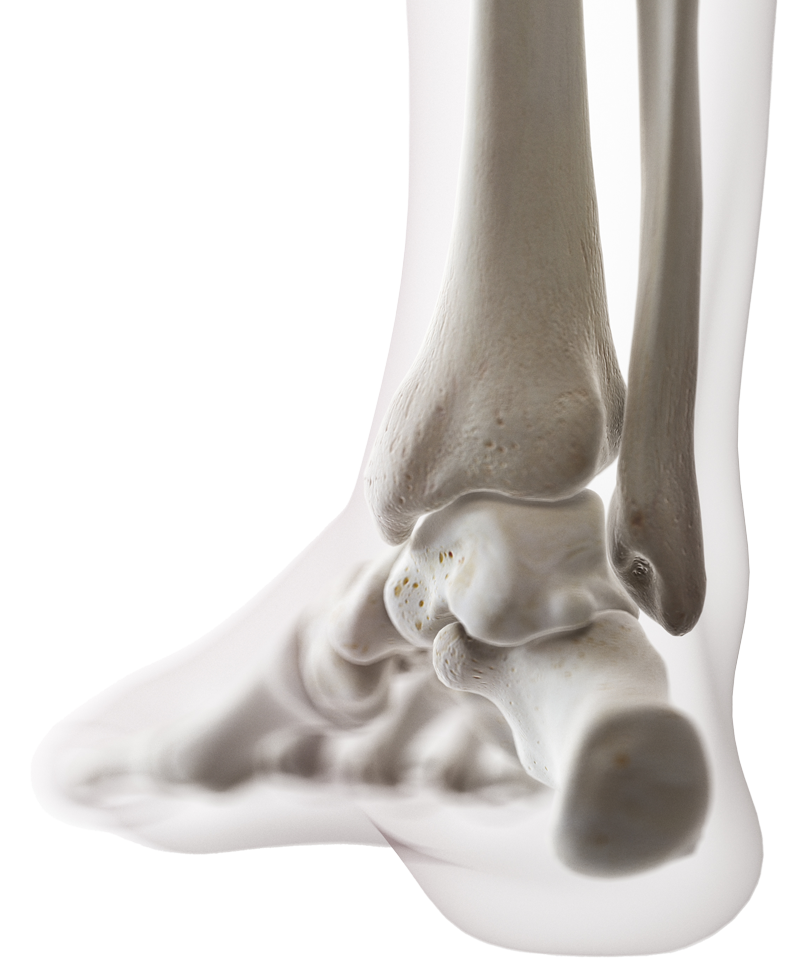
Mechanism Of Injury
A twisting injury or going over on the ankle usually results in an inversion of the foot and ankle. This produces a spectrum of injuries to the lateral ankle. These injuries very commonly occur in running sports such as soccer, basketball and netball. Depending on the severity of the injury, disruption begins with rupture of the anterolateral ankle joint capsule in milder injuries, followed by the anterior talofibular ligament (ATFL) and then the calcaneofibular ligament (CFL) becoming involved with more severe injuries. Isolated CFL rupture is possible without major injury to the ATFL. This occurs when there is an inversion injury with the ankle in a neutral or dorsiflexed position.
Thus a bad ankle sprain results in tearing or rupture of the lateral ligaments (ATFL and CFL). These ligaments will heal but they heal with the ligaments in a stretched position. This causes the ankle joint to feel sloppy and increases the risk of the patient going over on the ankle in the future. Every time you go over on the ankle the ligaments may stretch a bit more and render the ankle more unstable. There is also a risk of damaging the ankle joint surface every time you go over on the ankle.
Most ankle sprains (80%) recover completely with conservative treatment. Chronic ankle symptoms following a sprain may be due to either or both of the following sources: (1) residual symptoms from ankle joint pathology - ankle instability, chondral or osteochondral (joint surface) injuries in the ankle, anterior ankle impingement, posterior ankle impingement; (2) injuries to structures around the ankle joint - peroneal tendon tear, peroneal tendon subluxation or dislocation, fracture of the anterior process of calcaneus, lateral process of talus fracture, fracture of the base of the 5th metatarsal.
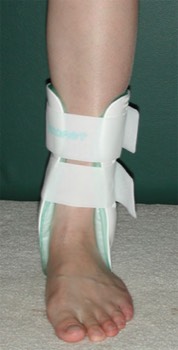
Fig 1. Ankle brace
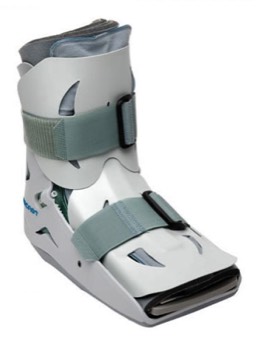
Fig 2. Short walker boot
Recurrent Ankle Sprains
The patient will give a history of recurrent sprains. The ankle feels weak and they do not trust their ankle and have a feeling of instability. They will have difficulty walking on uneven terrain. There is discomfort with manoeuvres that involve sudden starting and stopping motion and pain with push off activities such as running. They may also have pain and swelling with increased activity.
If recurrent ankle sprains are left untreated then this will lead to the development of ankle arthritis. The ankle arthritis usually develops over a 20 to 30 year period. As recurrent ankle instability usually starts when the patients are in their 20s, the painful arthritis usually presents when the patients are in their late 40s or early 50s. The current treatment for painful ankle arthritis is either ankle fusion or ankle replacement. Thus it is much better to prevent the development of ankle arthritis with ankle lateral ligament reconstruction.
Unstable Ankle Management
Active rehabilitation is the mainstay of treatment for chronic ankle instability. This involves physiotherapy that concentrates on soft tissue massage, range of motion exercises, peroneal muscle strengthening and proprioceptive retraining. Bracing (Fig 1) may be helpful.
If you continue to have instability despite a 2-3 month trial of physiotherapy treatment then surgery is indicated. The aim of the operation is to restore the length (i.e. shorten) of the elongated anterior talofibular and calcaneofibular ligaments. The surgery can be performed as a day surgery procedure. The surgery is done through a small incision about 2 cm long. Following the surgery, you may be able to weight bear in an ankle brace for 2 weeks followed by a short walker boot (Fig 2). The ankle brace needs to be worn for the first 2 weeks after the surgery.
Physiotherapy commences two weeks post operatively. This allows a more rapid return to function and sports. You may start light jogging at 6 weeks post op. The use of a plaster cast can delay rehabilitation and return to activities.
For specific advice regarding ankle instability, please book an appointment with Dr Peter Lam on (02) 9884 9499.